Interstitial Lung Disease | Vibepedia
Interstitial lung disease (ILD), also known as diffuse parenchymal lung disease (DPLD), encompasses a broad spectrum of over 200 distinct conditions that…
Contents
Overview
The concept of interstitial lung disease didn't emerge as a singular entity but rather as a growing recognition of a pattern of lung pathology distinct from common conditions like bronchitis or pneumonia. Early descriptions of diffuse lung scarring date back to the late 19th century, with physicians like Carl Friedrich Wilhelm von Rokitansky noting widespread fibrotic changes in autopsy specimens. However, it wasn't until the mid-20th century that a more cohesive understanding began to form, spurred by advancements in radiology and pathology. The term 'interstitial' itself gained traction as researchers like Averill Abraham Liebow meticulously classified these diverse conditions based on their microscopic appearance, distinguishing them from diseases primarily affecting the airways or blood vessels. The establishment of the American Thoracic Society (ATS) and the European Respiratory Society (ERS) in the mid-20th century provided crucial platforms for collaborative research and standardization of diagnostic criteria, solidifying ILD as a major category of pulmonary illness.
⚙️ How It Works
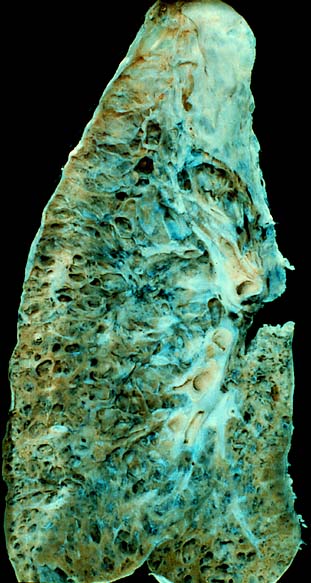
At its core, interstitial lung disease disrupts the delicate architecture of the lung's gas exchange units. The interstitium, a complex matrix of cells and extracellular material, normally supports the thin walls of the alveoli and the surrounding capillaries, facilitating efficient oxygen uptake and carbon dioxide removal. In ILD, various insults—ranging from inhaling inorganic dusts like silica and asbestos to systemic autoimmune diseases like rheumatoid arthritis—initiate an inflammatory cascade. This inflammation, if persistent, triggers myofibroblasts to deposit excessive collagen and other extracellular matrix proteins, leading to fibrosis. This scarring stiffens the lungs, reducing their compliance and capacity, and thickens the alveolar-capillary membrane, creating a physical barrier that impedes diffusion. The result is a progressive loss of lung function, often described as a 'honeycomb lung' in advanced stages, where the normal lung tissue is replaced by cystic spaces.
📊 Key Facts & Numbers
The prevalence of interstitial lung diseases is estimated to affect between 1.3 and 3.0 million people in the United States alone, with idiopathic pulmonary fibrosis (IPF) being the most common and aggressive form, typically diagnosed in individuals over 50. Globally, ILD represents a significant cause of respiratory morbidity and mortality, though precise figures are challenging due to the sheer diversity of subtypes and diagnostic variations across regions. For instance, sarcoidosis, another form of ILD, has a higher incidence in Northern European populations. The economic burden is substantial, with annual healthcare costs for IPF in the US alone estimated to exceed $10 billion, factoring in hospitalizations, medications, and supportive care. Survival rates vary dramatically by subtype; IPF patients have a median survival of only 3-5 years post-diagnosis, whereas some connective tissue disease-associated ILDs may have a more favorable prognosis.
👥 Key People & Organizations
Key figures in understanding and combating ILD include Dr. Averill Abraham Liebow, whose pathological classifications in the 1950s and 60s laid the groundwork for modern ILD diagnosis. More recently, researchers like Dr. Talmadge E. King Jr. at the University of California, San Francisco have made significant contributions to understanding IPF pathogenesis and treatment. Organizations such as the Pulmonary Fibrosis Foundation and the LUNGevity Foundation play critical roles in funding research, raising public awareness, and supporting patients and their families. Pharmaceutical companies like Gilead Sciences and Boehringer Ingelheim are at the forefront of developing novel therapies, investing heavily in clinical trials for antifibrotic and anti-inflammatory agents. The American Thoracic Society (ATS) and the European Respiratory Society (ERS) continue to set clinical practice guidelines and foster international collaboration.
🌍 Cultural Impact & Influence
The cultural resonance of interstitial lung disease often lies in its insidious nature and the profound impact it has on an individual's ability to engage with the world. Stories of individuals struggling with breathlessness, unable to perform simple daily tasks or participate in activities they once loved, highlight the disease's devastating effect on quality of life. Media portrayals, though less common than for diseases like cancer or heart disease, often focus on the patient's journey of diagnosis, the uncertainty surrounding prognosis, and the emotional toll on both patients and caregivers. Documentaries and personal memoirs frequently emerge, sharing intimate experiences of living with conditions like IPF, emphasizing themes of resilience, the search for effective treatments, and the importance of community support. The disease's impact extends to the healthcare system, influencing the development of specialized pulmonary rehabilitation programs and the increasing use of lung transplantation as a last resort for select patients.
⚡ Current State & Latest Developments
The current landscape of ILD management is dynamic, marked by a growing understanding of disease heterogeneity and the development of targeted therapies. In 2014, the approval of pirfenidone (Esbriet) by the FDA and subsequently by the EMA marked a turning point, offering the first drug shown to slow disease progression in IPF. This was followed by the approval of nintedanib (Ofev) in 2014, another tyrosine kinase inhibitor with antifibrotic properties. Research is rapidly expanding into novel therapeutic targets, including those involved in aberrant fibroblast activation, inflammatory pathways, and genetic predispositions. The American Thoracic Society's 2026 International Conference, for instance, featured presentations on machine learning for improved ILD diagnosis and new therapeutic agents, signaling a proactive approach to tackling these complex diseases. Organizations like Trevi Therapeutics are also exploring treatments for related conditions, such as pruritus in systemic sclerosis.
🤔 Controversies & Debates
A significant controversy in ILD revolves around the precise definition and classification of certain subtypes, particularly the distinction between idiopathic forms and those clearly linked to specific exposures or connective tissue diseases. The diagnostic challenge is immense; differentiating between various ILDs often requires a multidisciplinary approach involving pulmonologists, radiologists, and pathologists, and even then, a definitive diagnosis can be elusive, leading to the 'idiopathic' label. Another area of debate concerns the optimal timing and selection criteria for lung transplantation, a procedure with limited donor availability and significant post-operative risks. Furthermore, the high cost of newly approved antifibrotic medications like pirfenidone and nintedanib raises concerns about accessibility and equity in treatment, particularly in resource-limited settings. The exact role of environmental exposures, such as air pollution and specific occupational dusts, in triggering or exacerbating ILD remains an active area of epidemiological research.
🔮 Future Outlook & Predictions
The future of interstitial lung disease treatment is poised for significant advancement, driven by a deeper understanding of molecular pathways and the promise of personalized medicine. Gene sequencing and advanced imaging techniques are expected to enable earlier and more accurate diagnoses, potentially identifying individuals at risk before significant lung damage occurs. The development of novel antifibrotic agents, including those targeting specific c
Key Facts
- Category
- science
- Type
- topic