Psoriasis | Vibepedia
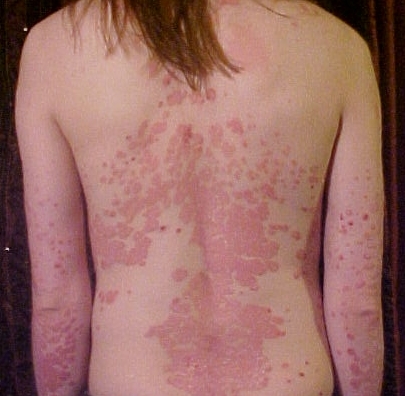
Psoriasis is a chronic, non-contagious autoimmune disease that manifests as distinct skin lesions, primarily characterized by red, itchy, and scaly patches…
Contents
- 🎵 Origins & History
- ⚙️ How It Works
- 📊 Key Facts & Numbers
- 👥 Key People & Organizations
- 🌍 Cultural Impact & Influence
- ⚡ Current State & Latest Developments
- 🤔 Controversies & Debates
- 🔮 Future Outlook & Predictions
- 💡 Practical Applications
- 📚 Related Topics & Deeper Reading
- Frequently Asked Questions
- References
- Related Topics
Overview
The history of understanding psoriasis stretches back millennia, with early descriptions often conflating it with other skin ailments. Ancient Greek physicians, including Hippocrates, noted skin conditions that likely encompassed psoriatic symptoms, though the term 'psoriasis' itself, derived from the Greek word 'psora' meaning 'itch', was first systematically applied by the Roman physician Galen in the 2nd century AD. For centuries, treatments were largely empirical and often ineffective, ranging from topical applications of tar and sulfur to more invasive methods. The true nature of psoriasis as an autoimmune disease began to emerge in the late 19th and early 20th centuries, with researchers like Louis-Anne-Jean Brocq and Paul Gerson Unna contributing to its classification and understanding of its cellular pathology. The pivotal shift occurred in the latter half of the 20th century with the advent of immunomodulatory therapies, transforming the management of this persistent condition.
⚙️ How It Works
At its core, psoriasis is an immune-mediated disease driven by a dysregulation of the immune system, particularly involving T-lymphocytes. In individuals with psoriasis, these T-cells mistakenly identify healthy skin cells as foreign invaders and trigger an inflammatory response. This leads to a rapid proliferation of keratinocytes, the primary cells in the epidermis, shortening their normal 30-day lifecycle to a mere 3-4 days. The resulting accumulation of immature skin cells, along with inflammatory cells and blood vessels, forms the characteristic psoriatic plaques. These plaques are often covered by silvery-white scales, which are essentially dead skin cells. The inflammatory cascade also involves cytokines like TNF-alpha and interleukins (IL-17, IL-23), which are key targets for modern biologic therapies developed by pharmaceutical giants like AbbVie and Janssen Pharmaceuticals.
📊 Key Facts & Numbers
Psoriasis affects an estimated 125 million people globally, representing about 2-3% of the world's population. In the United States alone, approximately 7.5 million individuals live with psoriasis, with an estimated annual healthcare cost exceeding $11 billion. The most common form, plaque psoriasis (psoriasis vulgaris), accounts for about 90% of cases, typically presenting as well-demarcated erythematous plaques with silvery scales, often on the elbows, knees, scalp, and trunk. Guttate psoriasis, characterized by small, drop-like lesions, often appears suddenly after a streptococcal infection. Pustular psoriasis, rarer and more severe, involves pus-filled blisters, while inverse psoriasis affects skin folds. Erythrodermic psoriasis, the most widespread and potentially life-threatening form, can cover the entire body.
👥 Key People & Organizations
Key figures in psoriasis research include James G. Krueger, whose work at The Rockefeller University elucidated the central role of the IL-23/Th17 pathway in psoriasis pathogenesis, leading to the development of targeted biologic drugs. Organizations like the National Psoriasis Foundation (NPF) in the US and the Psoriasis Association in the UK play crucial roles in advocating for patients, funding research, and raising public awareness. Pharmaceutical companies such as Novartis, Eli Lilly, and Amgen have been at the forefront of developing and marketing innovative treatments, including small molecule inhibitors and monoclonal antibodies, significantly altering the therapeutic landscape.
🌍 Cultural Impact & Influence
The cultural resonance of psoriasis, though often understated, is profound. For centuries, skin conditions have carried social stigma, and psoriasis is no exception. The visible nature of the plaques can lead to feelings of shame, isolation, and self-consciousness, impacting social interactions and mental well-being. This has led to patient advocacy groups and influencers, like those on Reddit forums and Instagram, to champion body positivity and destigmatize the condition. Media portrayals, while sometimes sensationalized, are slowly evolving to reflect the lived experiences of individuals with psoriasis, moving beyond mere physical description to acknowledge the psychological and systemic burdens. The rise of social media platforms has empowered patients to share their stories, fostering a sense of community and collective resilience.
⚡ Current State & Latest Developments
The current therapeutic landscape for psoriasis is rapidly evolving, marked by the increasing sophistication of biologic therapies and the emergence of oral small molecule inhibitors. Drugs targeting specific cytokines like IL-17A (e.g., secukinumab, ixekizumab) and IL-23 (e.g., guselkumab, tildrakizumab) have demonstrated remarkable efficacy and improved safety profiles compared to earlier broad immunosuppressants. The development of JAK inhibitors, such as upadacitinib, offers new oral treatment options. Furthermore, research is increasingly focusing on the gut microbiome and its potential role in modulating immune responses in psoriasis, with studies exploring the impact of probiotics and dietary interventions.
🤔 Controversies & Debates
A significant debate revolves around the optimal treatment strategy for moderate-to-severe psoriasis: biologics versus oral small molecules. While biologics offer high efficacy, their parenteral administration and cost can be barriers. Oral JAK inhibitors provide convenience but carry potential risks of infection and malignancy that require careful monitoring. Another ongoing discussion concerns the long-term management of comorbidities associated with psoriasis, such as cardiovascular disease and metabolic syndrome. There's also controversy regarding the accessibility and affordability of newer treatments, with patient advocacy groups frequently highlighting issues of insurance coverage and high co-pays, particularly in the United States healthcare system.
🔮 Future Outlook & Predictions
The future of psoriasis treatment points towards even more personalized medicine, leveraging genetic profiling and biomarkers to predict individual responses to specific therapies. Research into the role of the microbiome is expected to yield novel therapeutic targets, potentially leading to microbiome-modulating treatments. Gene therapy and advanced cell-based therapies are also on the horizon, though likely further out. The focus will continue to expand beyond skin clearance to addressing the systemic inflammation and associated comorbidities, aiming for holistic patient well-being. Experts predict a continued decline in the prevalence of severe, debilitating disease as treatment options become more effective and accessible, with a greater emphasis on early intervention and prevention strategies.
💡 Practical Applications
While psoriasis is primarily managed through medical treatments, practical applications of understanding its mechanisms extend to lifestyle modifications and supportive care. Patients are often advised on stress management techniques, as stress is a known trigger for flare-ups. Dietary interventions, though not a cure, are explored for their potential to reduce inflammation, with some individuals finding benefit from anti-inflammatory diets rich in omega-3 fatty acids and antioxidants, as recommended by organizations like the Arthritis Foundation. Phototherapy, using controlled exposure to ultraviolet light, remains a viable treatment option, often administered in clinical settings or through home-use devices. Patient education platforms, such as those provided by the National Eczema Society (though focused on eczema, their patient-empowerment models are relevant), offer crucial guidance on skincare, medication adherence, and coping strategies.
Key Facts
- Year
- 2nd century AD (first systematic description)
- Origin
- Ancient Greece/Rome
- Category
- science
- Type
- topic
Frequently Asked Questions
What exactly causes psoriasis?
Psoriasis is an autoimmune disease where the immune system, specifically T-cells, mistakenly attacks healthy skin cells. This triggers an inflammatory response that causes skin cells to grow too quickly, typically in 3-4 days instead of the normal 30 days. This rapid buildup of immature skin cells, combined with inflammatory cells and blood vessels, forms the characteristic red, scaly plaques. While genetics play a significant role, environmental factors like stress, infections (such as strep throat), and certain medications can also trigger or worsen flare-ups. The exact trigger for the immune system's misdirection remains a subject of ongoing research by institutions like the National Institutes of Health.
Is psoriasis contagious?
No, psoriasis is not contagious. It is an autoimmune condition, meaning the body's own immune system is involved, not an external pathogen like a virus or bacteria that can be transmitted. You cannot catch psoriasis from someone else through casual contact, sharing personal items, or any other means of transmission. This distinction is crucial for reducing the stigma associated with the condition, as it is not a public health risk in terms of transmissibility, unlike infectious skin diseases such as ringworm or impetigo.
What are the main types of psoriasis?
There are five main types of psoriasis. Plaque psoriasis (psoriasis vulgaris) is the most common, accounting for about 90% of cases, presenting as raised, red patches with silvery scales, often on the elbows, knees, and scalp. Guttate psoriasis appears as small, drop-shaped lesions, often triggered by a bacterial infection. Inverse psoriasis affects skin folds like the armpits and groin, appearing as smooth, red patches. Pustular psoriasis is characterized by pus-filled blisters and can be localized or widespread. Erythrodermic psoriasis is the most severe, causing widespread redness and scaling that can cover the entire body and is considered a medical emergency.
Can psoriasis be cured?
Currently, there is no known cure for psoriasis. It is a chronic condition that requires long-term management. However, treatments have become highly effective at controlling symptoms, reducing inflammation, and achieving long periods of remission where skin clears up significantly. The goal of treatment is to manage the disease, improve quality of life, and prevent or treat associated health problems. Advances in biologic drugs and small molecule inhibitors have revolutionized psoriasis management, allowing many patients to achieve clear or nearly clear skin.
What are the long-term health risks associated with psoriasis?
Psoriasis is more than just a skin condition; it's a systemic inflammatory disease linked to several serious comorbidities. Individuals with psoriasis have an increased risk of developing psoriatic arthritis, which causes joint pain, stiffness, and swelling. They are also at higher risk for cardiovascular disease, including heart attack and stroke, due to chronic inflammation. Other associated conditions include type 2 diabetes, inflammatory bowel disease (like Crohn's disease), obesity, and mental health issues such as depression and anxiety. Regular monitoring and management of these comorbidities by healthcare providers, often in conjunction with specialists like rheumatologists, are crucial.
How is psoriasis treated?
Treatment for psoriasis aims to reduce inflammation, slow skin cell growth, and remove scales. Options range from topical treatments like corticosteroids, vitamin D analogs, and retinoids, to systemic medications such as methotrexate and cyclosporine. Phototherapy, using controlled exposure to UV light, is also effective. For moderate to severe cases, biologic drugs (injected or infused) that target specific parts of the immune system, like TNF-alpha, IL-17, or IL-23, are highly effective. Oral small molecule inhibitors, such as JAK inhibitors, offer another convenient treatment option. The choice of treatment depends on the severity and type of psoriasis, as well as the patient's overall health and preferences, often guided by dermatologists at centers like Mayo Clinic.
What is the Koebner phenomenon in psoriasis?
The Koebner phenomenon, also known as the isomorphic response, is a characteristic feature observed in psoriasis where skin injuries can lead to the development of new psoriatic lesions at the site of trauma. This means that cuts, scrapes, sunburns, or even surgical incisions can trigger psoriatic plaques to appear in those specific areas. This phenomenon highlights the role of skin integrity and immune response in the manifestation of psoriasis. It's important for individuals with psoriasis to be mindful of potential skin trauma and to protect their skin to minimize the risk of inducing new lesions through the Koebner phenomenon.